From Heartburn to Regurgitation: Acid Reflux vs. Bile Reflux
Last updated on April 11th, 2025 at 05:56 pm
Are you feeling that burning sensation in your chest after every meal? Or perhaps you're experiencing a bitter taste in your mouth and frequent throat clearing? You might be dealing with acid reflux or bile reflux. While both conditions share similar symptoms, it's important to understand their key differences to get the right diagnosis and treatment. Get ready, and let’s dive into understanding acid reflux vs bile reflux and learn what you need to know for better management.
Acid Reflux vs. Bile Reflux
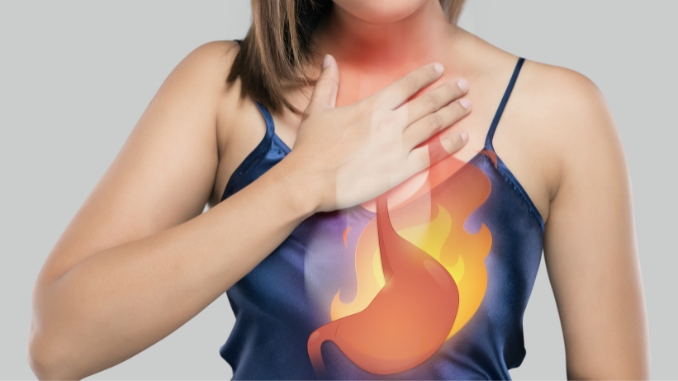
Bile and acid reflux are conditions involving abnormal digestive fluid movement but differ in the specific fluid involved.
Acid reflux appears when the lower esophageal sphincter (LES) doesn't close properly. This permits acid to travel back up into the esophagus. Gastric acid is often treated with proton pump inhibitors to reduce acid production.
Bile reflux, on the other hand, is when bile—a digestive liquid produced in the liver and stored in the gallbladder—flows backward from the small intestine into the stomach and even up into the esophagus. This can happen due to issues like surgery that alter the anatomy of the digestive system or due to malfunctioning valves.
Unlike gastric acid reflux, bile reflux involves fluid consisting of bile, which can be more damaging to the esophagus. Both conditions can also lead to inflammation of the esophagus (esophagitis) if left untreated.
Causes and Risk Factors
The causes of acid and bile reflux can vary, but some common factors can increase the risk of developing these conditions.
Acid Reflux
Main Cause
Malfunctioning lower esophageal sphincter (LES). As explained, the acid flows back into the esophagus when the LES fails to close properly.
Risk Factors
1. Hiatal Hernia
The stomach pushes up through a hole in the diaphragm, in a hiatal hernia protrudes into the chest through the diaphragm.
This anatomical abnormality can weaken the lower esophageal sphincter at the bottom of your esophagus that connects it to your stomach. The weakened LES allows stomach acid to flow back into the esophagus, contributing to acid reflux.
2. Obesity
Excess body weight, particularly around the abdominal area, can exert increased pressure on the stomach. This pressure may force stomach contents, including acid, into the esophagus, leading to acid reflux signs.
3. Pregnancy
During pregnancy, the growing uterus can press against the stomach, altering the normal position of the organs in the abdominal cavity. This physical change can also weaken the LES, facilitating the upward movement of stomach acid, causing or exacerbating acid reflux symptoms.
4. Smoking
Smoking has been linked to the weakening of the LES. Additionally, it encourages the production of stomach acid, making smokers more susceptible to acid reflux.
5. Certain Foods and Drinks
Consuming specific foods and beverages can worsen or trigger acid reflux symptoms. Spicy or acidic foods, chocolate, caffeine, and alcohol are known culprits. These items can also relax the LES or directly irritate the esophageal lining, contributing to the reflux of stomach acid.
6. Lying Down After a Meal
Reclining or lying down too soon after eating hinders the normal process of gravity aiding digestion. This can permit stomach acid to flow back into the esophagus more easily, contributing to acid reflux symptoms.
7. Eating Large Meals
Overeating can distend the stomach, increasing pressure on the LES. This heightened pressure makes it more likely for stomach contents, including acid, to reflux into the esophagus.
8. Certain Medications
Some treatments, such as calcium channel blockers, antihistamines, and sedatives, can relax the LES, making it less effective in preventing the backflow of stomach acid into the esophagus.
Bile Reflux
Main Cause
It is a malfunctioning pyloric valve. Bile can flow back into the stomach and esophagus if the valve doesn't close properly.
Risk Factors
1. Gastric Surgery
Procedures that alter the normal anatomy of the digestive system, particularly gallbladder removal surgery (cholecystectomy), can disrupt the usual flow of bile. Without the gallbladder, bile may flow more freely into the small intestine and even into the stomach, leading to bile reflux.
2. Complications from Peptic Ulcers
Peptic ulcers, open sores that form on the lining of the stomach or duodenum, can lead to bile reflux as a complication. The breakdown of tissue caused by ulcers may disrupt the normal containment of bile in the small intestine.
3. Intestinal Disorders
Conditions affecting the small intestine, such as Crohn's disease or bacterial overgrowth, can increase the risk of bile reflux. These disorders may disrupt bile's normal movement and flow through the digestive system.
4. Certain Medications
Some medications used to relax the smooth muscle of the digestive tract can contribute to bile reflux, such as sedatives and opioids. This relaxation of the muscles may allow bile to flow in the incorrect direction, leading to reflux symptoms.
5. Peptic Ulcer Surgery
Surgical interventions to treat peptic ulcers may alter the normal flow of bile, potentially causing it to reflux into the stomach and esophagus.
It's important to note that both acid reflux and bile reflux can occur independently or coexist, and their causes and risk factors may overlap.
Symptoms of Acid Reflux
Symptoms of acid reflux encompass a range of discomforts, including heartburn, a burning sensation in the chest typically after meals or when lying down, regurgitation of stomach contents leading to a sour taste, intense chest pain often mistaken for heart issues, difficulty swallowing due to esophageal irritation, chronic nighttime cough, hoarseness, persistent sore throat, laryngitis, asthma-like symptoms like wheezing and breathing difficulties, and occasionally increased salivation as a response to acid irritation. T
hese symptoms highlight the complexity of acid reflux and the need for effective management to improve well-being and prevent complications.
Symptoms of Bile Reflux
Unlike acid reflux, symptoms of bile reflux encompass various discomforts.
Including a burning sensation in the chest or upper abdomen, persistent nausea with an urge to vomit, vomiting that may include yellow or green bile, upper abdominal pain, a bitter or sour taste due to bile regurgitation, a sensation of fullness in the upper abdomen even with small meals, chronic cough resulting from airway irritation, generalized discomfort or indigestion marked by bloating and belching (dyspepsia), potential inflammation of the esophagus causing pain and difficulty swallowing (esophagitis), and in severe cases, unintended weight loss.
Recognizing these specific symptoms is vital for distinguishing between bile and acid reflux and guiding appropriate treatment choices.
When to See a Doctor
While occasional episodes of acid or bile reflux may be common and can often be managed with lifestyle changes and over-the-counter medications, as well as bile acid sequestrants, there are certain situations where it's important to seek medical attention.
If you experience constant or worsening symptoms despite making lifestyle changes and using over-the-counter medications or bile acid sequestrants, it's advisable to consult with a healthcare professional.
They can help specify the underlying cause of your signs and recommend suitable treatment options, including powerful acid-suppressant medications like ursodeoxycholic acid.
Additionally, if you experience severe chest pain, difficulty swallowing, unintentional weight loss, or if your symptoms are interrupting your daily activities and quality of life, it's essential to seek medical attention promptly.
A healthcare professional can execute a thorough evaluation, conduct diagnostic tests if necessary, and develop a personalized treatment plan to effectively manage acid and its complications—bile reflux gastritis or esophageal cancer.
Furthermore, if bile reflux is diagnosed, specific approaches for treating bile reflux may involve addressing excess acid production, surgical interventions like gastric bypass surgery, or other medical strategies to treat bile reflux and avoid further damage to the stomach lining. Accurate diagnosis of bile reflux is crucial to initiate the most appropriate treatment plan.
Conclusion
Acid and bile reflux are common digestive issues with overlapping symptoms, making it crucial to differentiate between them for proper diagnosis and treatment.
Understanding the causes, risk factors, and symptoms of acid vs bile reflux enables collaboration with healthcare experts to create an effective management plan. This can include lifestyle adjustments, dietary changes, medications, and occasionally surgery, all contributing to improved digestive health and a higher quality of life.
From now on, you no longer have to live with the dire consequences of poor digestion. You can finally obtain “gut health security” and enjoy your favorite foods, symptom-free all day long! So check out this 14-Day Digestive Health Quick Start Program now!
Rick Kaselj MS, is a leading kinesiologist and injury specialist as well as co-creator of the best-selling Unlock Your Hip Flexors program. Rick creates exercise programs that help people heal injuries and eliminate pain, so they can go back to living a full, active, healthy life.